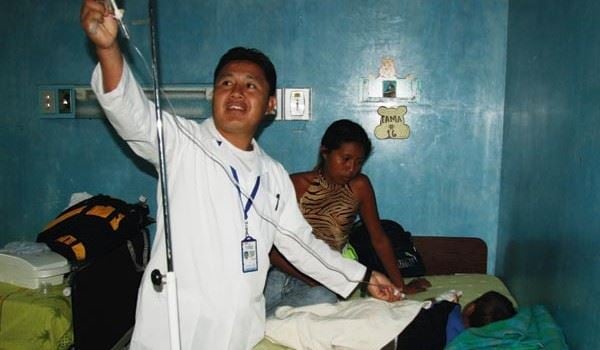
High-humidity rainforest grows only a few kilometres from the simple but immaculately clean room to which a worried mother has brought her sick child. Between the walls painted in the colours of the tropical sky, in the very heart of Venezuela, Florencio Morillo stands ready for action. The young man belongs to the Amazonian Yekuana tribe. Although he is neither a doctor nor a nurse, the long course he has taken to become a heath worker may mean the difference between life and death for the youngest members of his village.
According to a recent report, specially trained laypeople like Florencio are reducing infant mortality all over the world. The international report was published in March, and it
includes expert contributions from Norway’s National Knowledge Centre for the Health Services and from SINTEF.
The report provides up-to-date information about what the world has gained by training individuals to become health workers – training in which Norway’s ‘humanitarian ambassador’ Mads Gilbert, among others, has been involved.

Florencio Morillo has neither diploma nor degree, but a spell at the local hospital is part of the training that has turned him into a “barefoot doctor” in Venezuela.
Photo: Inger Scheel
Click to open
Focus on public health
In 2007, Gemini wrote about the ‘Jungle University’, a system set up in mine-infested areas by doctors Gilbert, Hans Husum and Torben Wisberg, where laypeople are trained as first-aid auxiliaries and ‘barefoot surgeons’. The three doctors have documented that this form of training saves a large number of land-mine victims from the loss of life and limb. Three years ago, researchers in Oslo obtained funding to go through all the research available on the effects of lay workers’ efforts in the health sector, with the idea of finding out what were the effects, if any, of their efforts on public health in different countries. The report is based on a study of 82 research projects, and shows that lay health workers have reduced mortality in children under five years of age in countries such as Ethiopia and Tanzania. They may well also have reduced rates of serious infections in childhood in India and Nepal, to name but two countries.
The most powerful result is the link between the use of lay health workers and maternal/child health, when such workers are employed in vaccination programmes and when they provide breastfeeding advice. The report also shows that specially trained lay health workers have improved people’s chances of being cured of tuberculosis.
“Ideologically, however, there is a wide range of opinions regarding lay health workers; some people place them on a pedestal, while others are more inclined to pull them down,” says chief scientist Inger Scheel of SINTEF Technology and Society.
But first: Where do we find lay health workers, and what do they do?
A buffer for authorities?
A shortage of doctors and nurses has led several countries and organizations to offer special training to lay people so that they can work in the health sector – knowledge that will enable them to offer preventive care, perform simple treatments and recognize symptoms that require the patient to be referred to more qualified personnel.
Lay medical personnel are a well-known feature of low- and medium-income countries in Asia, South America and Africa. But they are also used in poor districts in industrialized countries such as the USA, not to mention in wealthy Norway, where the ‘Breastfeeding Aid’ organization is an example.
“What most of these people have in common is that they are put into service in their own local community, either as part of the public health service or through voluntary organizations,” explains Inger Scheel.
“The health workers give the neighbourhood a feeling of greater independence and ability to cope.”
Research Manager Odd-Geir Lademo
Major study of lay health workers
The lack of professional health personnel is a threat to public health in low- and middle-income countries.
Eleven per cent of the population on the planet suffer from a quarter of the world’s health problems, but have access to only three per cent of the world’s healthcare personnel.
This was the background of a recent study to which the National Knowledge Centre for the Health Services and SINTEF made important contributions.
The study performed a systematic survey of 82 research projects that had been done in order to shed light on the effects of the efforts of specially trained lay health workers.
The work was financed by the Research Council of Norway, and the results have been published by the internationally respected Cochrane Library database.
For many years, Scheel and her fellow researchers at SINTEF and the Knowledge Centre have been following lay health workers at close hand. It was Scheel who gave us
Florencio’s story. When the photo was taken, he had received practical training at the hospital in the provincial capital of Amazonas State in Venezuela. Now he has completed his training, and is a “barefoot doctor” in state employment. But does he deserve to be glorified, or not?
Scheel says there are conflicting ideological views about lay health workers.
“Some people regard these workers as virtual liberators, as individuals who can perform a range of important functions that extend beyond their purely medical tasks. This
is based on a perception that such lay personnel help local communities to take control of their own situation because they are no longer helpless when they are hit by illness or accidents; yes, that these health workers give whole neighbourhoods a feeling of coping and of greater independence,” says the chief scientist, before adding, “Others claim that lay health workers can act as a protective buffer for the authorities, or are held hostage by them because they make it acceptable to use low-paid health sector workers, and that the system undermines efforts to educate doctors and nurses locally.”
Promising approach
We meet Scheel on her home ground at SINTEF in Oslo, surrounded by the signs of spring outside her office window. Late winter has been a busy season for her and her colleagues Claire Genton and Gloria Azalde, who have joined us.
Scheel and Glenton contributed to the report on lay health workers, for which Simon Lewin of the Knowledge Centre was primarily responsible. They were interested in building a picture of what lay health workers can mean for public health among all groups of people. However, the 82 studies that they found were limited to the efforts of lay workers in poor countries and among the less well-off in rich countries such as the USA.
In the wake of the publication of the report, the three SINTEF researchers and Lewin made a trip to Venezuela, one of the leading countries in the use of lay health personnel.
“Is it true that specially trained lay persons always strengthen the health service system?”
“Some of the 82 studies showed no effects, but most of them documented that the efforts of lay personnel have resulted in improvements in health, though to different degrees. So my answer would be that using lay health workers is a promising approach,” says Scheel.
“Is it cost-effective to use lay personnel in the health sector?”
Senior researcher Claire Glenton answers: “For another report, we went systematically through studies that looked at the cost-effectiveness of the lay personnel vaccination programme, but we found very little material. I think that little research has been done in this area.”
In the wake of revolutions
As they travelled through Venezuela, the Norwegian researchers interviewed two types of lay personnel: first, “barefoot doctors” like Florencio, who work full-time for the Ministry of Health. They have the authority to write prescriptions for 46 medicines and they also visit schools, where they provide information about preventing AIDS and on contraception. The other group of interviewees only give vaccinations.
The list of interviewees also included representatives of national and local health authorities. The purpose of the trip was to gain a better understanding of how political systems and social change are affecting the survivability of health services that employ lay personnel, explains Scheel.
“We had already done similar interviews in South Africa. Both Venezuela and South Africa have been through revolutions, so we have two pre-revolutionary societies to look to, and two that have been shaped by drastic change.”
“So what have you found?”

With her refrigerated bag of vaccines, this young unqualified health worker is ready for another spell of duty at a health station in the Venezuelan Andes.
Photo: Inger Scheel
Click to open
“We have to keep some of our results confidential until we have published them, but this much we can say. In Venezuela, President Chavez has written it into the Constitution that everyone has a right to full and free healthcare. To implement this, he has very rapidly built up a parallel heath system staffed by Cuban doctors. When the range of health services is supposed to be identical for everyone, it is easy for people to begin to regard lay health workers as a second-class option, so we are keen to see what will happen there,” says Scheel.
Proud health workers
As they face us across the table in Oslo, the researchers enthusiastically describe Venezuelan health stations that are staffed by lay personnel. They are small but well-equipped clinics with immaculately clean rooms, homemade posters, shelves and pill-boxes covered with tissue paper, and homemade artificial flowers. On the walls hang hand-drawn maps of the area, with each individual house drawn in.
“We met vaccinators, who were greeted sceptically by professional nurses at first, but who now feel that they are valued members of the team. And they are very proud of the
job that they do,” says Gloria Azalde, who shows us her favourite quote from an interview with one of the lay workers: “Now I am so fully accepted as a vaccinator that when
children who are to be vaccinated see me, they start crying.”
“You also mention negative reactions to lay personnel in the health service. Is there any clear answer to the question of whether such people bring benefits or otherwise?”
Inger Scheel does not take long to answer: Locally recruited health workers can bring local communities non-medical benefits to a quite different degree than those who come from outside of the area. One important aspect is the feeling that a village or city district can manage on its own. Such people also have the best linguistic background for the job. It is unrealistic to expect that enough doctors can be trained to cover every little corner of huge areas of rough country in places such as Venezuela or South Africa. In any case, it would hardly be sustainable to pay a doctor to sit in a remote village with 20 inhabitants, waiting for one of them to fall ill.
Svein Tønseth